According to the World Health Organization, 20–33% of people worldwide live with painful musculoskeletal diseases, and musculoskeletal diseases are the second leading cause of disability[1].
This situation forces doctors to look for new ways to treat such diseases. One of them is intra-articular plasma lifting, or autoplasmotherapy (in accordance with the nomenclature of medical services approved by Order of the Ministry of Health of Russia dated October 13, 2022 No. 804n - intra-articular administration of drugs). In simple terms, this is treatment with your own blood plasma. The method not only helps relieve pain, it relieves inflammation, improves joint mobility and accelerates the process of restoration of cartilage tissue in it.
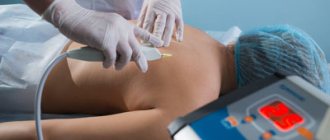
Reinfusion of autologous blood Reinfusion of autologous blood into the joint area can help combat pain and inflammation. More details
Plasmolifting technology was developed relatively long ago and was initially used in dentistry, but in the course of research conducted by Russian doctors, it turned out that the patient’s own plasma can work in almost any tissue of the body. Thus, plasma lifting entered the arsenal of traumatologists and orthopedists[2].
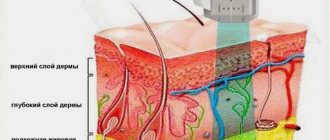
The essence of plasmolifting is that the patient’s platelet-rich blood plasma (PRP) is injected into the damaged areas of the joints. Cartilage tissue has a very weak ability to regenerate independently, especially in older people, and the introduction of plasma starts the recovery process - treatment is much faster and more effective. Platelets contain biologically active substances that stimulate healing processes, the so-called growth factors. They activate fibroblasts - connective tissue cells located in the deep layers, causing them to actively synthesize elastin, collagen and hyaluronic acid. As a result, the patient’s microtraumas heal, blood supply improves, pain decreases, joints become more mobile, and the process of restoring the structure of bone tissue at the site of cracks begins.
Plasma is injected directly into the joint itself, which means that the method works in a targeted manner without affecting other tissues and organs. Another feature of plasmolifting is that it uses the restorative resources of the body itself, is completely hypoallergenic and does not cause the side effects that can occur during drug therapy.
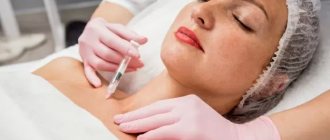
Treatment of arthrosis of the knee joint Intra-articular administration of drugs can be used in the treatment of arthrosis of the knee joint. To learn more
In addition, the plasma lifting procedure is minimally traumatic. Despite the fact that the method is injection, there is practically no pain during the procedure, and there is no need for subsequent rehabilitation of the patient. Literally the next day after the injection, a person can return to their usual lifestyle.
We recommend reading:
- Plasmolifting in orthopedics and traumatology
- Plasmolifting in the treatment of the spine
- Plasmolifting of joints
- Plasmolifting of the knee joint
- Plasmolifting: how many procedures are needed
- Recommendations before the plasma lifting procedure
- Plasmolifting for arthrosis
- Plasmolifting for coxarthrosis
- Plasmolifting for arthritis
- Plasmolifting for osteochondrosis
- Plasmolifting how much does 1 procedure cost?
- Plasmolifting preparation for the procedure
- Plasmolifting of the hip joint
- Plasma therapy for the treatment of joints
More articles →
Principle of the method
The PRP method in the treatment of knee joints is based on enhancing the regeneration of intra-articular tissues. Thanks to platelet-rich plasma, cartilage, menisci, ligaments and other tissues are restored faster.
Even in ancient times, doctors drew attention to the fact that traumatic injuries accompanied by the formation of a hematoma heal much faster. The reasons for this have been established only in recent decades. It turned out that platelets secrete a number of substances that accelerate regeneration. These are the growth factors:
- epidermal;
- epithelial growth;
- endothelium;
- fibroblasts;
- insulin-like;
- transformative.
These substances have a polypeptide (protein) structure. They have different purposes. But all of these compounds take part in tissue regeneration. They stimulate the mitotic activity of cells, accelerate their growth and division.
PRP therapy for the knee joint makes it possible to significantly increase the intensity of reparative processes of both soft and bone tissues. In medicine, platelet-rich plasma is increasingly used. It is used for any injuries: soft tissue damage, muscle and ligament ruptures, bone fractures. All types of tissues regenerate faster if a sufficient number of platelets are present.
Why do they contact us?
- No queues
No need to wait, we work by appointment
- All in one day
Doctor's appointment, diagnosis and treatment on the day of treatment
- Let's relieve the pain
We relieve pain in just 1-2 visits to us
- We guarantee
Professional approach, affordable prices and quality
- Doctor's appointment 0 RUB!
If the cost of treatment is more than 30,000 rubles
- Three treatment options
We will select several methods and offer optimal treatment
What is this?
PRP is platelet-rich plasma. The patient's own plasma is used during the treatment process. It is prepared from autologous blood immediately before injection into the knee.
Platelets are the formed elements of blood that perform the function of forming a blood clot. By gluing, they initially form a “plug” in damaged vessels. This happens immediately after the injury. Then platelets provide their surface for the formation of the main reactions of plasma blood coagulation.
Not long ago, another important function of platelets was established. It turned out that they secrete a large number of growth factors and take part in regenerative processes.
Normally, the concentration of platelets in the blood ranges from 180 to 360 thousand cells per μl. Even this amount is enough to somewhat speed up the regenerative processes. But they occur faster and more intensely if a lot of platelets are injected into the joint. Therefore, the plasma is pre-prepared. Other formed elements of blood are removed from it. The platelet concentration increases 5 or more times.
It has been established that the maximum regenerative potential of tissues is achieved when they are exposed to plasma containing at least 1 million platelets per 1 μl. Further increases do not provide significant benefits. If the platelet count exceeds 1.8 million, inflammatory reactions may be enhanced. Therefore, too high a concentration of these cells is not recommended for use for intra-articular administration.
What are the contraindications?
The method uses a person’s own plasma, which makes the method highly safe - allergic reactions, infection with hepatitis, HIV and other infections are excluded. In addition, there are no side effects that can develop when using medications. However, there are contraindications to treatment:
- Local skin infections in the injection area
- Acute infectious diseases
- Pregnancy
- Coagulation disorders (relative contraindication)
Price
On the one hand, the cost of the procedure is low, since the only thing needed is a centrifuge, an ultrasound machine, and inexpensive instruments. The “bottleneck” is the presence of a doctor who can quickly and accurately perform an injection into the area of the intervertebral disc. It is also quite a fashionable and popular technique, and the price can be quite high.
On average, the cost of one session in Moscow starts from 4,000 rubles, and may well reach the upper mark of 9,000 rubles. At the same time, the high cost does not guarantee that all the rules for plasma preparation and patient preparation will be followed. Typically, the price depends on competition, the flow of patients to the clinic, service, rental or ownership of premises, and the location of the clinic.
In large cities of Russia prices are lower, but not always:
- Saratov, at ArthroMedCenter: 2350 rubles per session;
- Volgograd,: plasma therapy session – 2500 rubles;
- Krasnodar, prices at the Euro LPS clinic: 4,000 rubles per session.
How do they do it?
Blood is taken from the patient from the cubital vein. He then waits for 20 minutes for the intra-articular injection. During this time, the drug is prepared. Centrifugation is used. It can be one- or two-stage. In the first case, it is possible to better preserve the integrity of platelets, in the second, their higher concentration is obtained.
After preparing PRP, the resulting plasma is administered intra-articularly. The injection site is numbed with an anesthetic. Therefore, the patient does not feel significant pain during the procedure. In terms of tolerability, it can be compared to an intramuscular injection - unpleasant, but quite tolerable.
Some patients feel a feeling of fullness inside the joint. Especially in cases where a large volume of plasma is administered. After the injection, the doctor asks the patient to perform flexion and extension movements in the knee joint so that the plasma is better distributed in the joint cavity. After 10 minutes the patient goes home. He does not require hospitalization or additional observation.
Plasma can be used in courses of varying durations. Most often, PRP is administered once a week. A total of 3 to 7 injections are required. The treatment regimen is selected individually. The doctor forms it based on the clinical situation and the purposes of using platelet-rich plasma.
Indications
Among knee joint diseases, the following diseases and conditions are considered indications for the use of PRP:
Arthrosis of the knee joint or gonarthrosis. A degenerative disease associated with the gradual degradation of articular cartilage. The use of PRP at stages 1-2 can improve regenerative processes in cartilage tissue. Thanks to this effect, a significant slowdown in the development of the pathological process is achieved. With the help of PRP, doctors are able to eliminate many symptoms of arthrosis, delay the need for knee replacement, or even abandon the operation completely if an effective conservative therapy regimen is used, in which PRP is one of the elements.
Injuries. The knee is often injured by athletes. Most often these are ligament ruptures and meniscus damage. Intra-articular fractures occur. If the doctor determines that conservative treatment is sufficient, he or she may use PRP to speed up the healing of the lesions. Otherwise, they can take a very long time to recover. This process takes weeks, or even months.
Operations. After arthroscopic surgery on the knee, a rehabilitation period follows. It continues until all tissue damage is restored. PRP can be used to speed up this process.
Defects of the articular surface. PRP is used for cartilage deficiency of articular surfaces of any origin. The cause may be injuries, arthrosis, inflammatory diseases of the knee, metabolic pathologies, psoriasis, systemic connective tissue lesions and other diseases. With a small defect, it is possible to enhance the regenerative processes of PRP. If there is a significant area of cartilage thinning, surgical treatment is indicated.
After operation
PRP knee therapy is used after ligament and meniscus surgery. There are many studies demonstrating the effectiveness of this procedure for accelerating the recovery of intra-articular structures.
One common area of application remains rupture of the anterior cruciate ligament of the knee. She herself cannot fully recover from a complete rupture. Therefore, to normalize its fusion (ligamentization), surgical treatment is used. Free autografts are used.
There are different types of them. STG (intrinsic tendon) and BTV grafts (“bone-tendon-bone”) are used. In both the first and second cases, the introduction of PRP into the knee allows one to achieve significant positive treatment results.
First of all, PRP is performed to speed up the rehabilitation period. Studies show that when using STG grafts, the ligamentization period is on average 369 days (about 1 year), while the use of PRP reduces this period to 177 days (6 months). That is, the terms are reduced by 2 times.
Even more significant results can be achieved when using PRP therapy for the knee after using a VTV graft to reconstruct the anterior cruciate ligament. The average time for ligamentization is about 1 year. When using PRP it was possible to reduce it to 3.5 months.
Studies demonstrate that ligamentization after surgery is significantly better in patients receiving PRP therapy than in the control group. True, the results are better only 4-6 months after surgery. The examination of patients after 1 year shows that the final results are the same.
However, PRP therapy can significantly reduce the recovery time for patients after surgery. This is especially important for professional athletes who want to return to training as quickly as possible.
Effectiveness for arthrosis
When to expect results depends on the purpose of using PRP and the indications for treatment. In any case, it does not develop instantly. PRP is not a pain reliever. Platelet-rich plasma only enhances tissue regeneration, and this process takes quite a long time.
For arthrosis of the knee joint, the maximum effect develops 3-6 months after the start of treatment. Only a few patients report a decrease in pain after the first injection. For others, the first results are achieved within a month from the start of therapy.
In comparative studies, PRP shows much better results than intra-articular glucocorticoids. These differences are especially noticeable in grade 3 gonarthrosis. Pain syndrome in patients with this method of treatment is less pronounced. In addition, PRP has a more beneficial effect on cartilage - plasma stimulates its regeneration, while glucocorticoids, on the contrary, have a chondrotoxic effect.
According to E.Kon, 80% of people were satisfied with the results of the treatment after a series of injections of platelet-rich plasma for osteochondrosis. Results were assessed after 5 weeks. Another study found that treatment results were rated as positive by 67.3% of patients six months after undergoing PRP therapy for knee arthrosis. In the control group this figure was only 4.3%.
Another study calculated the average amount of time that elapses from the first injection until the therapeutic result is obtained. Patients considered this to be a reduction in clinical symptoms. This period was 17.63 days.
It should be noted that PRP has two main effects: anti-inflammatory and reparative. When surveying patients, only short-term symptomatic effects are taken into account. It develops more quickly after administration of platelet-rich plasma, but goes away more quickly after completion of the course of therapy. The first results of treatment are due to hyperplasia of the synovial membrane and modulation of the level of cytokines in the articular cavity.
At the same time, the main effect of PRP is chondrogenesis. But this process is happening too slowly. Patients cannot feel it. Only by comparing the symptoms and radiological parameters of the main and control groups are researchers able to obtain data on the effectiveness of PRP therapy for the knee joint several months after the course of treatment.
Advantages and disadvantages, complications
The benefits indicate the significant safety of this treatment for patients. This is complete compatibility between the administered substance and the patient, since everything that is administered to a person is taken from him. Accordingly, there is no risk of infecting the patient with HIV infection or viral hepatitis through blood. The plasma lifting session has a prolonged effect and does not require daily repetitions.
Own blood components, unlike non-steroidal anti-inflammatory drugs, do not harm the gastrointestinal mucosa. Finally, there is no allergy and no harmful systemic effects.
Despite all the advantages, the method is invasive; the needle must be brought as close as possible to the affected intervertebral disc. In fact, if we slightly change the operating factor, and do not inject platelets, but use a laser LED, then we already get a modern minimally invasive neurosurgical intervention.
There is a certain danger of infection of medical personnel, although the patient is usually not concerned about this disadvantage. If the patient has a blood pathology, thrombocytopenia and thrombocytopathy, hemorrhagic syndrome, then this method cannot be used.
There are no optimal data on platelet concentrations, and modern randomized trials have not yet been able to show a precise correlation between clinical effects and platelet concentrations. There are also difficulties in preparing plasma, in which red blood cells can get into the finished injection material. They are equivalent to hemorrhage into the joint cavity, causing inflammation and increased pain. It is also required to comply with the parameters of two-stage centrifugation, and maintain time and speed conditions. If you reduce the time and speed during centrifugation, then in the supernatant layer, which is collected for the second stage, there will be a lot of leukocytes and erythrocytes, which will worsen the result.
The most common complication is the occurrence of pain when the patient is injected with activated plasma, which contains a large amount of released platelet-derived growth factors. Pain in the affected vertebra can last up to several days. The therapeutic and protective regime, wearing a corset, helps relieve pain. Compresses, distracting and cooling ointments, and short-term use of non-steroidal anti-inflammatory drugs are used.
Also, unfortunately, it is impossible to exclude local soft tissue abscess and infiltration associated with a violation of the procedure for introducing the material. There may also be a hematoma, which, however, quickly resolves and does not bother the patient for long.